This article was first published on Discover Society, November 2014.
Last June, a group of Italian MPs proposed jail terms and fines for authors of so-called “pro-ana” (anorexia) and “pro-mia” (bulimia) websites. These are self-styled online communities on eating disorders which are viewed as promoting extreme dieting and unhealthy eating practices. France and the United Kingdom preceded Italy’s attempt to pass restrictive legislation as far back as 2008-9, and many internet service providers also endeavoured to ban these contents.
But the potential spread of health-hazardous behaviours is probably only one side of the coin, and these websites might also channel health-enhancing assistance, advice, and support (Yeshua-Katz & Martins 2013). In fact a closer look reveals that website users carefully manage their online socialisation to address their health challenges. Online social spaces enable discussion around the illness and constitute a complement, albeit an admittedly imperfect one, to formal healthcare services. There is no rejection of standard health norms in the name of some extreme ideal of thinness but rather a need – or perhaps, a cry – for extra support.
A social science approach brings out these results. The effect of web interactions on health does not only depend on website contents, but also on how people actually use them, share them, and access resources through them. The social, rather than just clinical dimension of eating disorders, recognized long before the advent of the web (Bell 1985, Orbach 1978), becomes ever more relevant in the current context and calls for a more comprehensive view of the “ana” and “mia” social universe.
Four Types of Support
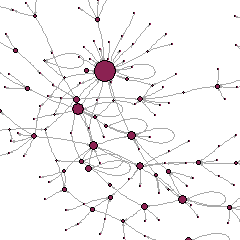
As part of the 4-year ANAMIA research project, conducted with a team of researchers in France and Britain, I fielded an online survey of users of these websites, to elicit information on their social relationships (personal networks) both online and face-to-face, and their health support networks for two types of issues, “serious” such as hospitalization, and “mundane” such as hair loss. The latter distinction aimed to illuminate the specific types of support that are sought in each case, following House’s (1981) classical typology differentiating between informational support (information, advice for health decision-making), emotional support (empathy, affection, trust and encouragement), instrumental support (material services, practical and financial assistance), and companionship support (a sense of belonging, not being lonely).
Not unexpectedly, our data show that demand for these different forms of support depends on the type and severity of problems experienced: for minor issues, guidance and advice (informational support) usually suffice, while more serious concerns also require empathy, listening, understanding (emotional support) and even material help (instrumental support).
More interestingly, an article I co-authored with a fellow ANAMIA project researcher (Tubaro & Mounier 2014) finds that persons with eating disorders activate different parts of their personal network of acquaintances and friends according to the type of support they need. Specifically, ana and mia online groups provide distinct sources of support, especially for minor issues that primarily require information and guidance: indeed content sharing enables users to draw on peers’ knowledge and experience. These groups offer freedom of expression, action and decision, without depriving their members of a sense of community (companionship support) that relieves and protects them. The presence of strong ties, that is, close or very close friends and contacts, is not necessary: weak ties, that is, acquaintances perceived as less close, or with whom interactions are infrequent, often suffice to access informational support.
Internet helped me a lot not to feel alone… because at the beginning of my eating disorder, well, I really felt alone. Nobody would understand me, and all that… with Internet, I realized I was not alone, I was not the only one experiencing this.
We created a [..] blog […] to post all American studies on the topic […] We put a name on an illness and many people said, ‘Ah, this is what I have, and nobody takes me seriously.
[Two respondents, English- and French-speaking sample]
Personal Networks Matter

How ana and mia individuals enjoy these benefits depends on the structure of their personal networks. It is known in sociology that support, solidarity, and a sense of belonging appear in very cohesive social environments — dense personal networks, where all interact with all (Putnam 2000). However, cohesion also increases peer pressure on the individual to abide by the group’s norms, and any deviations are more likely to be detected, judged and even reprimanded. In scattered social environments (personal networks with few connections between individuals or between sub-groups), the individual retains greater freedom of action, but at the cost of less solidarity. A person with eating disorders must arbitrate between these two opposing needs, trying to access support to better manage the disorder every day, while minimizing social control and negative criticism.
I don’t want everyone to know, because I would feel observed when I go out.
[A respondent, French-speaking sample]
The preferred solution turns out to be to split one’s personal network into unconnected sub-groups, whereby web-based ana-mia communities constitute a separate social space with hardly any links to other contexts of interactions, whether online (generalist platforms like Facebook) or face-to-face (family, school, friends, etc.).
I am a different person on my blog and on Facebook. On Facebook, I am the one that everyone knows; on my blog, I am the one that nobody suspects.
It’s two different worlds, the forum and the others. The others are on Facebook. […] What separates these two worlds? They are not aware […] two different worlds that must not overlap.
[Two respondents, English- and French-speaking sample]
Managing Networks to Cope with the Disorder
Protection from unwanted disclosure of personal information is achieved by sharing one’s history of distress, or talking about symptoms, in an ana-mia forum whose members are not in any other social circle (family, school class,

sports team, church etc.). In keeping interaction contexts separate and presenting a different aspect of themselves in each of these contexts, individuals manage self-image and reputation, referring to multiple and sometimes very diverse social representations of health and nutrition.
Insofar as dedicated ana-mia sites remain separate from all other contexts of interaction, their members can reduce the overall social pressure exerted by their personal networks, while maintaining access to differentiated sources of support, and without giving up strong ties for weak internet ties. Persons with eating disorders do not completely hide information on their health status and eating practices, but manage it by deciding, on a case-by-case basis, what to reveal to whom.
This should not be interpreted as an escape from “real life”, so to speak, to find refuge in an “imaginary” online community; nor does it mean that ana-mia website users reject medical care to opt for peer support only. Rather, online communities constitute a surrogate solution when provision of healthcare from established providers is seen as inadequate or wanting – for example in the case of persons who are at an early stage of the illness, whose weight has not reached critical thresholds to need hospital treatment, or who live far from specialist healthcare centres.
They [doctors] need to know that … even those who are not … who are not thin or do not need emergency hospitalization are just as much in distress, and there are many suicide attempts because of that.
[One respondent, French-speaking sample]
The Potential and Possibilities of Internet Interactions
Rather than censoring online eating disorder communities, health policy-makers and care providers should rely on the potential and specificities of online interactions to reach out to a largely underserved population.
Online medical intermediation can be a matching form of care, relatively inexpensive and yet able to improve the daily life of persons with eating disorders, also including those who are undiagnosed, have only mild symptoms, or are otherwise excluded from specialized care services. Especially for information support, participation of health professionals can be combined with interaction between peers. The challenge is to strike a balance between the two, by strengthening the presence of the former without discouraging the active participation of the latter.
Such a service could be a space for interactions that users can easily keep separate from other social circles. In particular, the use of pseudonyms should be allowed, without demanding real names. Neither should access require authentication through users’ profiles on other online services (such as Facebook, Gmail, or Twitter). In this way, online interactions could reconcile different perspectives and really act to the benefit of sufferers — to finally move going beyond the moral panic around “pro-ana”.
References
Bell R. M. (1985). Holy Anorexia. Chicago: University of Chicago Press.
House J.S. (1981). Work, Stress and Social Support. Reading, Mass: Addison-Wesley.
Orbach S. (1978). Fat is a Feminist Issue. London: Arrow.
Putnam R.D. (2000). Bowling Alone: The Collapse and Revival of American Community. New York: Simon & Schuster.
Tubaro P. & Mounier L. (2014). Sociability and support in online eating disorder communities: Evidence from personal networks. Network Science, 2(1): 1-25.
Yeshua-Katz D. & Martins N. (2013). Communicating stigma: The pro-ana paradox, Health Communication 28(5): 499–508.